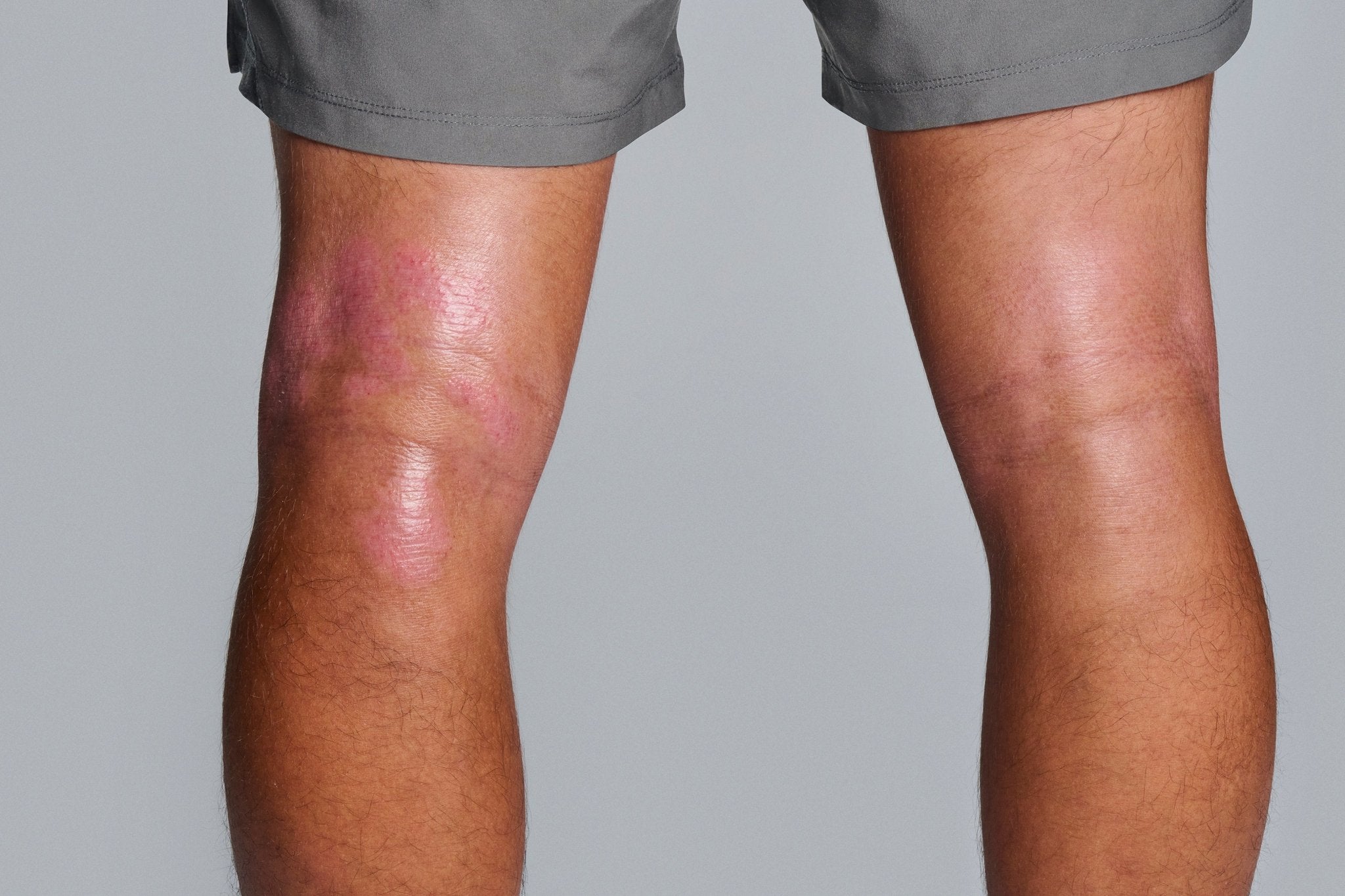
Finding a mysterious red patch on your skin is bad enough – but not knowing what it is? No way! Eczema and psoriasis are the two biggest culprits of scaly rashes, and they can be tough to tell apart. That’s why we want to clear up the eczema vs. psoriasis confusion once and for all, so you can say goodbye to uncertainty around treatment and the frustration of confusion. Let’s investigate!
What are the differences between eczema & psoriasis?
While these two itchy skin conditions may look the similar, they do have different causes, symptoms, and appearances that can help you differentiate between the two. There are also different variations of each skin condition to keep in mind, which can complicate diagnosis and treatment. We go into much more depth about each type of eczema here, but a brief overview of the forms of both psoriasis and eczema will help us better understand the differences between the two.
Types of eczema
- Atopic dermatitis - The most common form of eczema, this often appears in the creases of the knees and elbows and usually results in dry, red, and itchy skin.
- Contact dermatitis - As the name suggests, this form is caused by contact with a specific irritant or chemical and has more rash-like symptoms (such as blistering and hives) than other eczema types.
- Neurodermatitis - Very similar to atopic dermatitis, but it often appears in specific areas such as hands, feet, neck, and scalp, in the form of itchy and discolored skin (red, brown, or gray).
- Dyshidrotic eczema - Another form of eczema that causes blistering, this also lasts longer than typical eczema flare-ups and appears on palms of your hands, soles of your feet, and in between your fingers and toes.
- Nummular eczema - Likely the closest visually to psoriasis and ringworm, this type shows up as circular and scaly patches of red skin and can be anywhere on your body.
- Seborrheic dermatitis - Primarily found on oily parts of your body, this results in red, flaky areas of skin on the face, chest, and back.
- Stasis dermatitis - This is caused by poor circulation to your legs, which allows water and blood cells to pool there. Identified by swollen ankles, open sores on the feet or legs, and redness/discoloration of the skin.
Types of psoriasis
- Plaque psoriasis - By far the most common type of psoriasis, plaque psoriasis makes up 80-90% of cases. It causes raised patches of rough and red skin on the knees, elbows, and back that can crack and bleed.
- Inverse psoriasis - Very red and occasionally shiny patches in the folds of your body, often around the groin, knees, and elbows where the moisture in these areas usually prevents scaling and dryness of the patches.
- Pustular psoriasis - Appearing as redness followed by blisters or pustules, this type of psoriasis can be limited to certain areas of the body or be more widespread depending on the case.
- Guttate psoriasis - This type of psoriasis leads to inflamed, small, round, red spots that mostly appear on the legs, arms, and torso.
- Erythrodermic psoriasis - A rare form of psoriasis, this causes inflammation and pain across the majority of the body along with swelling and other serious side effects if left untreated. If you have an erythrodermic psoriasis flare-up, seek medical attention immediately.
Causes
Now that we have a baseline understanding of where and how eczema and psoriasis can appear on the body, we should look at why they show up in the first place. Both of these skin conditions are very complex and have many different causes and forms of treatments that should be discussed with a dermatologist to decide what’s best for your situation. However, having an overview of the potential symptoms and options can help you be more informed for when you do go speak with your doctor.
Eczema
There is no clear-cut cause of eczema (unfortunately). Most people with eczema do have higher levels of inflammation in the body from an overactive immune system, making that a likely culprit. Studies also show that some people with eczema have a mutation of the gene that causes filaggrin, the protein that forms the top protective layer of skin.
Last but not least, there’s staph A. (or scientifically, Staphylococcus aureus). Medical professionals and researchers used to see Staphylococcus aureus overgrowth in the skin microbiome as a symptom of eczema — from excess scratching and broken skin. Now, that’s all changing, and staph A. is thought to be the real trigger of eczema, rather than a byproduct.
Psoriasis
Psoriasis, on the other hand, is caused by rapid skin cell growth. This increased speed causes skin cells to build up and cause red, flaky patches. The exact cause of psoriasis is unknown, but genetics and triggers to the immune system like illness, stress, medications, allergies, or environmental factors are thought to play a role in the development and flare-up of psoriasis.
Symptoms
Itching
Let’s start with the basics: both eczema and psoriasis appear as itching red rashes. Sometimes, though, you can differentiate between the two by the type of itch. Psoriasis tends to be less itchy but can have a slight burn. Eczema, on the other hand, can have more severe itching. Some people with eczema will scratch so much it leads to broken skin.
Location
Both skin conditions can show up wherever, whenever they want, but psoriasis tends to be extra fond of the scalp, front of the elbows and knees, face, and buttock. Eczema is typically spotted on the back of the knees or in the crease of the elbows where sweat can build up and irritate the skin.
Appearance
Psoriasis and eczema may both show up as red rashes on the skin, but they do have notable differences in appearance. For example, psoriasis tends to have a silvery appearance, with a film of scaly skin overtop. It’s also thicker and more raised than eczema. Eczema will have a less defined, unraised patch of skin that can appear cracked, rough, and leathery. Eczema will also sometimes leak liquid through the skin, making it less likely to scale than psoriasis.
Treatment
When it comes to treating psoriasis and eczema, you have options for both. While there is some overlap, others can be quite different. Unfortunately, neither skin condition has a cure at this time.
Eczema
Heavy moisturizing creams
Dryness makes eczema and itching worse, which is why it’s important to use a daily moisturizer. You can easily find heavy moisturizing creams without doctor assistance at many retailers.
However:
These heavy creams can be uncomfortable to use, leaving your skin feeling sticky. The layer of unabsorbed cream can then wreck sheets and clothing. They’re also laden with preservatives, which are actually anti-bacterial and kill both the good and bad bacteria on the skin. At the end of the day, these creams are not truly therapeutic and can end up doing damage instead.
Hydrocortisone cream
The first treatment method most doctors will recommend for eczema is an over-the-counter hydrocortisone cream. It’s a steroid that helps calm down your body's immune system, which helps to reduce itching and inflammation. For severe eczema, prescription hydrocortisone creams are available.
However:
Hydrocortisone creams can cause side effects like stinging, redness, headache, and more. When stopping use, there’s also the risk of topical steroid withdrawal, which produces more unwanted symptoms.
Phototherapy
Ultraviolet, or UV, lights can also help keep the immune system from overreacting and causing chronic inflammation. It can reduce redness and itching in both adults and children, and is generally used for those with widespread eczema across large portions of their body.
However:
This can be a slow solution, as it requires multiple weekly treatments and it could take one to two months to start seeing results. In addition, if sun exposure is a trigger for your eczema, it will worsen your symptoms and should be avoided.
Lifestyle changes
Avoiding hot water, long showers, excess handwashing, as well as harsh soaps, laundry detergents, and cosmetics may improve eczema symptoms, as can applying a moisturizer daily. Read more about how small lifestyle changes can improve your symptoms of eczema here.
However:
While these adjustments may help minimize itching and flare-ups, they don’t address the underlying causes of eczema.
Stress reduction
Increased cortisol in response to stress can cause symptom flare-ups, which to be honest, just causes more stress. Finding time to relax and practice self-care is not only healthy for your overall wellbeing, but it may even help you find a breakthrough for your eczema!
However:
Stress can be difficult to control and reduction typically needs to be done on top of another type of treatment for optimal results.
Drugs that suppress the immune system
Your doctor may prescribe medications in the form of pills, or injections that help keep your immune system from overreacting. This treatment is typically reserved for moderate to severe eczema.
However:
Possible side effects include increased risk of infections, vomiting, upset stomach, increased risk of certain cancers, and more. Immunosuppressants aren’t long-term options, and even in the short-term, can pose serious risks.
Treat the root cause
The list of potential eczema treatments is endless because there are so many types of eczema, situations, and potential causes. What most eczema treatments fail to address, though, is the imbalance of the skin microbiome.
Gladskin Eczema Cream uses endolysin Micreobalance® (our patented smart protein) that works with your skin, instead of against it, to restore balance to the skin microbiome gently and effectively while moisturizing at the same time.
You also don’t have to worry about resistance or harsh ingredients. Gladskin Eczema Cream is free of steroids, fragrances, drying alcohols, preservatives, parabens, and sulfates. It’s clinically tested and safely formulated for anyone three months and up.
That means you can treat your eczema without any “buts.” Just results.
In fact, four out of five users experience reduced itch and redness associated with eczema, and you can too. Learn more here.
Psoriasis
Salicylic acid
Ointments and products containing salicylic acid can help to remove layers of “scales” that come along with psoriasis. It accomplishes this by causing the outer layer of the skin to shed and is also used to treat other skin conditions like acne. However, using too much of this should be avoided as it can lead to further irritation and redness.
Coal tar
While the name may sound unappealing to put on your body, coal tar is a popular ingredient used to help treat psoriasis. It’s made from coal and wood (including juniper and pine) and helps slow the growth rate of the skin cells that cause psoriasis. It’s been used for years to help alleviate itching, swelling, redness, scaling/flaking, and slows the process of skin cell growth. Similar to salicylic acid, this can also lead to additional inflammation if left on for too long or used too often. It can also stain fabrics and even hair, so make sure to be careful when using it.
Phototherapy
Like with eczema, UV lights can also help keep the immune system from overreacting and causing chronic inflammation. However, unlike eczema, sunlight is not a trigger for psoriasis and actually slows the growth of the affected skin cells. Even natural sunlight may improve psoriasis symptoms.
Hydrocortisone cream
This steroid cream may also help to reduce the itching and inflammation associated with psoriasis. Over-the-counter or prescription creams can be used depending on the severity of the condition.
Can you treat bacteria to help psoriasis?
You may then be wondering… Do bacteria play a role in psoriasis? Research is inconclusive; however, Staphylococcus aureus has been found in psoriasis patients. In one study, 46% of participants had pathogens on the skin, the most common of all being staph A.
Because Gladskin products work with your skin instead of against it to regain balance in your skin microbiome, you can use them whether you have eczema, psoriasis, rosacea, acne, or all of the above.
Balancing your skin microbiome and locking moisture into the skin are both crucial when considering skin health, no matter your skin condition.
If you don't have a microbiome imbalance, the products still work as safe, effective cleansers and moisturizers because they’re hypoallergenic, and free of fragrances, alcohol, and preservatives.
Can eczema become psoriasis?
Thankfully, nope! While many people wonder if eczema can become psoriasis and you may be too, there’s no need to worry. Eczema and psoriasis are two different skin conditions. There is one catch: it’s possible you could have both conditions at the same time. Luckily, it’s super rare for that to happen!
Understanding psoriasis vs. eczema
Determining the differences between eczema & psoriasis isn’t a straightforward process. With a little detective work and the help of a healthcare professional, you’ll be able to decipher the difference and find appropriate treatment. When in doubt, you can take measures to boost your skin health overall by using moisturizers, avoiding harsh cosmetic ingredients, de-stressing through lifestyle changes, and balancing and maintaining your skin microbiome with Gladskin.
Sources:
https://www.psoriasis.org/topical-treatments/
https://www.psoriasis.org/about-psoriasis/
https://stm.sciencemag.org/content/6/244/244ra90
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4211527/
https://nationaleczema.org/eczema/
https://eczema.org/information-and-advice/treatments-for-eczema/phototherapy/