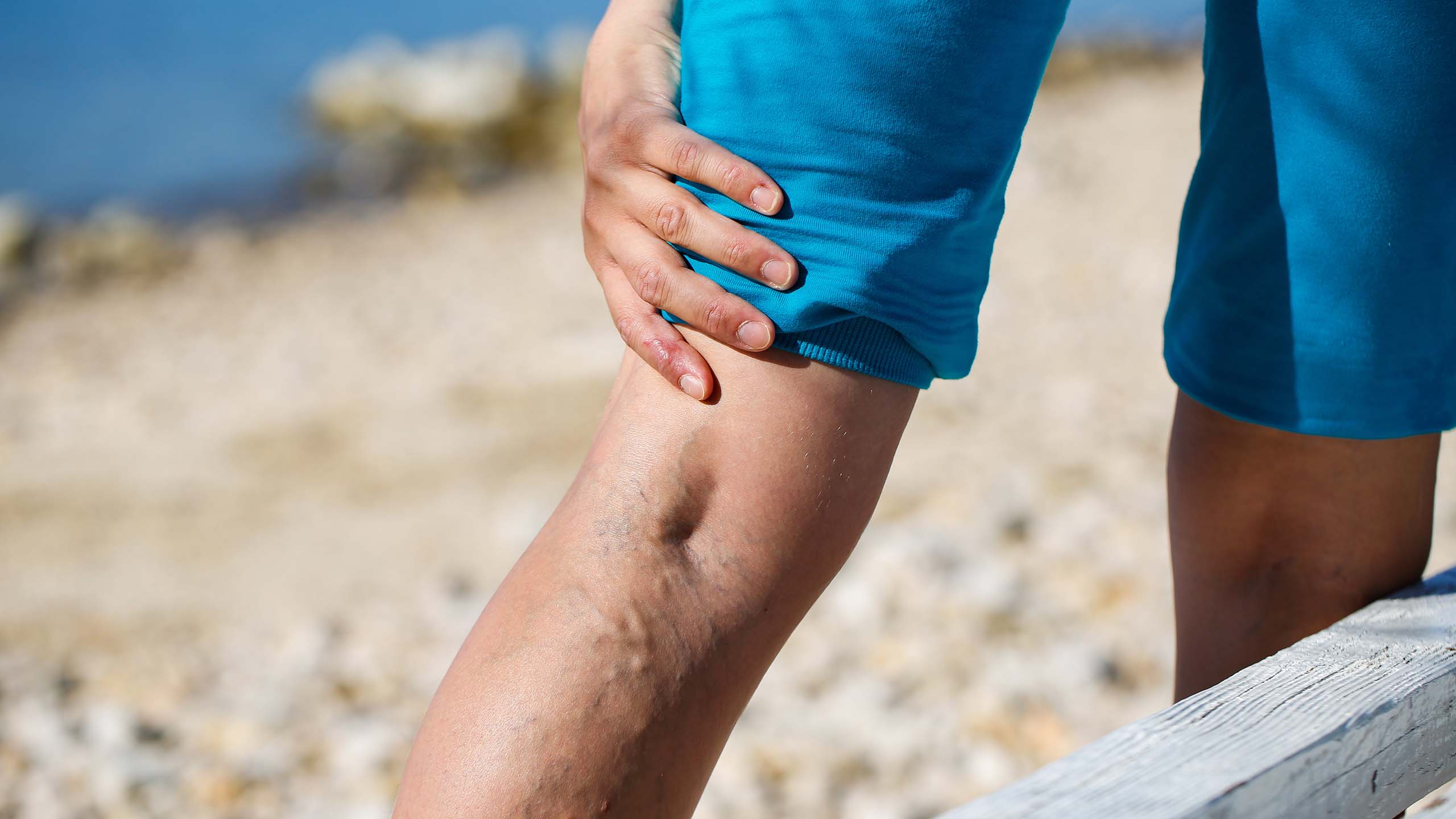
Stasis dermatitis is unlike any other form of eczema. Stasis dermatitis can result in itchy skin like most types of eczema but also is accompanied by swollen ankles and heaviness or aching at the end of a long day.
This form of eczema is sometimes referred to as gravitational dermatitis, venous eczema, and venous stasis dermatitis. Because it’s so different from any other type of eczema, let’s dive into exactly what stasis dermatitis is, what the symptoms are, what causes stasis dermatitis, and how to treat it.
What Is Stasis Dermatitis?
Stasis dermatitis is a chronic condition that can lead to everything from itchy skin to ulcers and swelling in the lower legs.
This condition results from insufficient blood flow and the pooling of water and blood cells in the lower legs, ankles, and feet.
Stasis dermatitis is more common in women than men and in those over 50 years of age.
Stasis dermatitis can indicate a significant underlying condition affecting your blood circulation, so it’s important to consult with your healthcare provider if you suspect you may have stasis dermatitis.
Stasis Dermatitis Symptoms
Stasis dermatitis symptoms can be divided into two categories: early symptoms and symptoms that appear later if the condition goes untreated.
The initial symptoms of stasis dermatitis include:
- Red, itchy skin on the legs, ankles, or feet (skin may look brown, purple, ashy, or gray on darker skin)
- Scaling or dryness
- “Cayenne pepper spots” or orange-ish, brown-ish specks on the skin
- Heaviness or aching after extended standing or walking
- Swelling of the lower legs, feet, or ankles on one or both sides (this is more common at the end of the day or after extended standing or walking)
As time passes, these symptoms may worsen if the stasis dermatitis and underlying venous insufficiency aren’t properly treated. New symptoms can also immerge, including:
- Venous ulcers (open sores) that may bleed, ooze, or scab
- Shiny skin that’s swollen
- Cracked skin
- Bumpy skin
- Thickened, hardened skin
Because stasis dermatitis can progress and worsen when left untreated, it’s crucial to not only manage symptoms but address the root cause of the skin condition.
What Causes Stasis Dermatitis?
Unlike most forms of eczema, researchers and medical professionals do know the root cause of stasis dermatitis. Stasis dermatitis occurs due to poor circulation (or venous insufficiency) in the lower legs. When you have venous insufficiency, the valves in your veins weaken and leak fluid. They no longer effectively push the blood back to the heart, and water and blood cells collect in the lower portion of the legs.
While venous insufficiency is often the root cause behind stasis dermatitis, it’s important to note that not everyone with venous insufficiency will then develop stasis dermatitis.
Poor blood circulation in the legs can result from natural aging. Still, it can also be caused by other underlying conditions that directly affect the blood, including deep vein thrombosis (or DVT), which involves a blood clot in the lower leg, varicose veins, congestive heart failure, kidney failure, high blood pressure, and injury or surgery to the lower legs.
Risk factors for stasis dermatitis not related to underlying conditions include:
- Being female
- Pregnancy and childbirth, especially multiple
- Being over the age of 50
- Being overweight
- Insufficient movement, including excessive standing or sitting
How to Treat Stasis Dermatitis
Treatment for stasis dermatitis aims to treat the root cause of venous insufficiency as well as manage symptoms, including swelling, itching, and aching.
If you believe you may have stasis dermatitis, schedule an appointment with your primary healthcare provider right away because this form of eczema can be an indication of underlying conditions that need attention.
From there, your doctor will provide you with guidance on how to address your venous insufficiency and manage the uncomfortable symptoms it can cause.
Your healthcare provider may suggest that you:
Wear Compression Stockings
Compression stockings help improve blood circulation and reduce swelling. If you’re unfamiliar with how compression stockings work, you’re in luck… they’re super easy to use!
Compression stockings look just like traditional socks, although they vary in length. You can find compression socks that fit just below the knee or all the way thigh-high.
These socks have been woven to distribute pressure at specific spots of the leg and enhance blood flow. Most doctors recommend putting your compression stockings on in the morning and taking them off before bed. However, always be sure to consult with your primary healthcare provider to get an expert recommendation for your unique condition.
Elevate Your Legs
Elevating your feet above your heart can also help relieve swelling in the ankles, feet, and lower legs that’s associated with stasis dermatitis.
Simply take breaks every two hours throughout your day to elevate your leg for about 15 minutes. You may also want to try elevating your legs while you sleep.
Avoid Excess Salt
Because excess salt in your diet can lead to increased water retention, you’ll want to avoid foods high in salt. Processed foods like canned or cured meats, frozen pre-made meals, salted nuts, pretzels, chips, canned soup, packaged ramen, and more tend to be higher in salt content.
To help you reduce your sodium intake and manage swelling, opt for fresh fruits and vegetables, unprocessed meats, and whole-food snacks.
Incorporate Movement Into Your Day
Long periods of standing or sitting can increase swelling in the legs, ankles, and feet. It can also cause you to feel heavy or achy.
To avoid this discomfort, incorporate movement into your day — whether that’s gentle stretching and a short walk or more rigorous exercise. Be sure to consult with your healthcare provider to establish what types of movement are best for your current state of health.
Take Care of Your Skin
Depending on the symptoms you’re experiencing on your skin and how far the stasis dermatitis has progressed, your healthcare provider may recommend a few different solutions to care for your skin.
If you’re really struggling with itchiness, your doctor may suggest an oral or topical antihistamine to make you feel more comfortable and prevent scratching. Scratching your rash may make your skin condition worse, and scratching may also increase your risk of infection if you scratch enough to cause lesions in the skin.
If you do have open wounds from scratching or because of ulcers and the skin becomes infected, your doctor will likely recommend an oral or topical antibiotic.
No matter what the current state of your skin health is, you should apply a moisturizer daily to help prevent drying skin and to support your skin’s natural protective barrier.
You’ll also want to avoid using harsh skincare products that contain preservatives, fragrances, dyes, parabens, sulfates, or other harsh chemicals. All of these common skincare ingredients can irritate the skin and make your stasis dermatitis worse.
Conclusion
Stasis dermatitis occurs due to poor circulation (or venous insufficiency) in the lower legs. While this can be caused by natural aging, venous insufficiency can also be indicative of an underlying condition.
If you’re experiencing any of the symptoms associated with stasis dermatitis, be sure to consult with your primary healthcare provider.
In the meantime, to help keep you comfortable, you’ll want to elevate your legs, incorporate gentle movement into your daily life, avoid excess salt, maybe try compression stockings, and take care of your skin by moisturizing and avoiding irritating skincare ingredients.