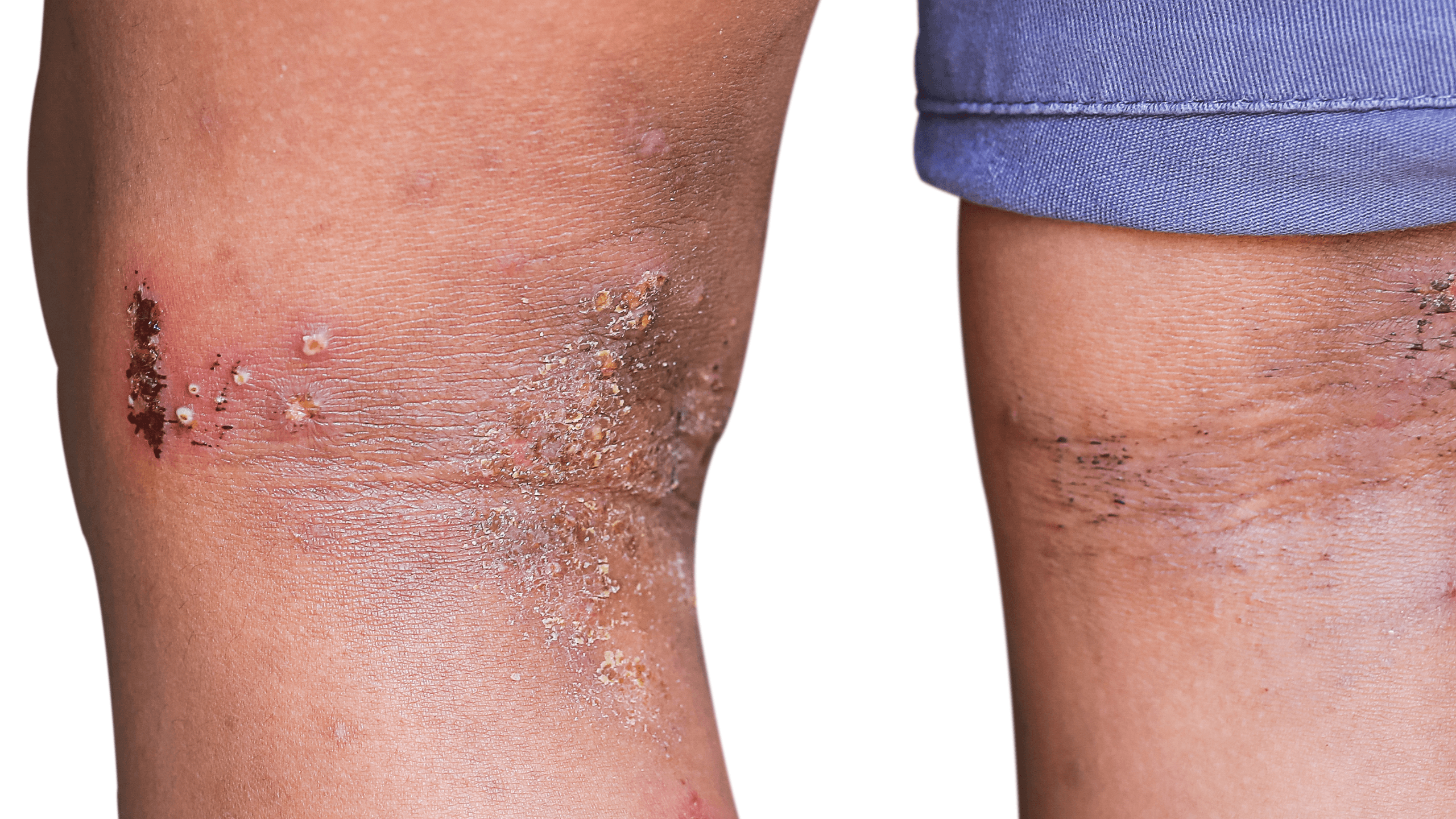
Your immune system and protective layers of skin are critical components in keeping your body safe. If you have a skin rash, skin that is warm to the touch, or redness and swelling of the skin, these could be signs your skin is inflamed and your body is fighting off environmental threats or internal infection.
What Is Skin Inflammation?
When your body begins to battle environmental threats, such as bacteria, viruses, allergens, or even wounds, your immune system activates, sending out inflammatory cells and cytokines in an attempt to heal the body and minimize the threat. This process results in inflammation, and it can take place anywhere in the body — including the skin. Inflammation is your body’s natural and beneficial way of protecting itself. It’s only when this inflammation becomes chronic that it poses a problem.
What Are the Symptoms of Skin Inflammation?
One of the main symptoms of skin inflammation is a rash. Inflammation-induced rashes can take many forms and have different characteristics, including:
- Burning or stinging
- Itching
- Redness
- Scaling of the skin
- Skin that is warm to the touch
- Pimples, blisters, or other small, red bumps
- Raised, thickened skin
- Cracks in the skin
What Causes Skin Inflammation?
Understanding the underlying cause of skin inflammation will help you to reduce inflammation long-term. Some reasons you may experience inflamed skin include:
Immune System Dysfunction
Sometimes your immune system becomes overactive and starts responding to things that aren’t real threats to the body. In the case of autoimmune conditions, the immune system actually starts to mistakenly attack your own healthy cells. This can lead to chronic inflammation. Autoimmune conditions that can affect the skin include lupus, psoriasis, and celiac disease.
For each one of these conditions, the immune system dysfunction manifests differently on the skin. People with celiac disease may notice red, itchy bumps after eating gluten. People with psoriasis experience red, scaly patches of thick skin that are extremely itchy.
Someone with lupus can experience rashes and sores that are often triggered by sunlight. A common sign of lupus also includes a red, butterfly-shaped rash over the face.
Although it’s not recognized as an autoimmune condition, eczema is an immune-modulated inflammatory disease. Experiencing the changes in skin color, flaking, and itchiness associated with eczema can also be an indicator of underlying immune system dysfunction.
Allergies
Allergic reactions to foods you’ve eaten, medications you’ve taken, or allergens you’ve come into contact with produce rashes on the skin.
If you’ve consumed a food or medication you’re allergic to, this will likely appear on the skin as hives. Hives cause red or skin-colored welts and itchiness.
When your skin comes into contact with an irritant or allergen, contact dermatitis can form. Signs and symptoms include a rash that can be red, brown, purple, or gray depending on your skin color, and that can often itch, sting, or burn. You could also have blisters. Common allergens that cause contact dermatitis are poison ivy, nickel, and latex.
Infection
Bacterial infections, viral infections, and fungal infections can all dramatically impact the skin. Infection occurs when foreign invaders, such as bacteria or viruses, enter the skin — usually through an open wound.
Possible skin infections include:
- Impetigo
- Cellulitis
- Ringworm
- Staph infections
- Athlete’s foot
Heat Rash
Heat rash develops when sweat can’t evaporate and instead clogs your pores. The perspiration trapped beneath the skin leads to inflammation and a red rash on white skin and gray or white on brown and black skin.
Photosensitivity
Photosensitivity occurs when your immune system reacts to the sun. This condition is also sometimes referred to as a sun allergy.
In people with photosensitivity, the body identifies standard changes in the skin due to sun exposure as threats and triggers an immune response. The reaction can occur due to UV rays from the natural sun or from a tanning bed. Photosensitivity can result from medications and some immune disorders, such as lupus.
Symptoms of photosensitivity often include an itchy rash that appears red on white skin and darker brown or black on brown and black skin. Photosensitivity sometimes also causes blistering and oozing.
How Is Skin Inflammation Diagnosed?
To accurately diagnose skin inflammation and its underlying cause, you’ll need to visit a healthcare provider. A doctor will likely begin by taking your medical history and then examining the skin to note external symptoms.
Oftentimes, inflammation caused by an infection can be diagnosed by a physical examination alone. If another cause is suspected, however, your doctor may need to ask further questions or complete various tests.
For immune system dysfunction caused by an autoimmune condition, your doctor may recommend blood tests.
If your doctor suspects an allergy, you may take a blood test as well as track eating habits and exposure to specific items in relation to the severity of your skin symptoms.
In some cases, your doctor may take a skin biopsy to evaluate the skin health on a microscopic level.
How to Treat Inflamed Skin
Treatment for inflamed skin may vary depending on whether you’re experiencing inflammation on the face or inflammation of the skin elsewhere on the body. It can also vary depending on the cause of the inflammation.
Topical Creams
Topical creams and ointments that are applied directly to the skin can help reduce skin inflammation. Different topical treatments for skin inflammation include:
- Antibacterial or antifungal creams for skin infections
- Corticosteroids to lower inflammation levels in the skin
- Immunomodulators like calcineurin inhibitors that influence the immune system
- Hydrocortisone cream to reduce itchiness
Oral Medications
Many different oral medications can also aid in the reduction of skin inflammation, including:
- Oral antibiotics or antifungals for skin infections
- Antihistamines for allergies
- Dapsone for hives
- Retinoids for psoriasis
Supplemental At-Home Remedies
While at-home remedies may not be the primary form of treatment for skin inflammation, they can act as a secondary treatment method to help reduce inflammation and manage symptoms more quickly. Some at-home remedies for skin inflammation include:
- Using a cool compress to soothe irritation. Simply run a clean washcloth under cool water, wring it out, and apply it to the skin.
- Applying a hypoallergenic, fragrance-free moisturizer to prevent cracked skin.
- Wearing loose-fitting, breathable clothing.
Addressing Skin Inflammation
Acute skin inflammation helps defend your body from infections and heal wounds. However, when skin inflammation becomes chronic, it can negatively affect your overall skin health. Depending on the underlying cause of skin inflammation, a doctor may recommend oral or topical treatments. To better understand why your skin may be inflamed and how to best treat it, visit your primary healthcare provider.